Author: Agnes LEUNG
Assistant Professor, Department of Paediatrics, CUHK
Food allergies are becoming more prevalent in our communities. In Australia, one in every ten young children is currently afflicted. Normally, your immune system protects you from pathogens and illness. It aids in the battle against bacteria, viruses, and other microorganisms that might make you sick. If you have a food allergy, your immune system wrongly perceives anything in a specific meal (most typically, the protein) as though it’s harmful to you. The dietary protein is known as an allergen, and your body’s reaction is known as an allergic reaction. A person with a food allergy produces an excessive amount of an antibody called IgE, which recognizes the offending food. When IgE and food come into contact, substances like histamine are generated, causing symptoms.
Responses might vary from mild skin rashes to life-threatening allergic reactions, known as anaphylaxis. Anaphylaxis is the most severe allergic response. It has a quick onset and might be fatal. Symptoms of a severe allergic response might appear minutes after being exposed to an allergen. In rare circumstances, the time frame following exposure might vary by several hours. Each reaction might be different in the same person. Anaphylaxis symptoms often include two or more of the following bodily systems: skin (hives, swelling of face, lip and tongue), respiratory (breathing difficulty, wheeze), gastrointestinal (vomiting, abdominal pain), and cardiovascular (pale complexion and collapse). Yet, a decrease in blood pressure without accompanying symptoms might also be indicative of anaphylaxis. It is also crucial to remember that anaphylaxis can develop without the appearance of hives. Someone who has previously experienced mild allergic reactions may suddenly suffer severe reactions that might be fatal. While fatalities are uncommon, anaphylaxis should always be treated as a medical emergency that requires rapid attention. Our recent local epidemiological data showed an increasing incidence of hospital and emergency department admissions for anaphylaxis between 2001 and 2019 among Hong Kong paediatric population,1, 2 which was consistent with observations from other developed countries such as Australia, Spain, United Kingdom, and United States.
More than 90% of childhood food allergies are caused by egg, peanut, tree nuts, cow’s milk, fish, shellfish, wheat, and soy. In Hong Kong, the most frequent food allergy triggers varied by age, with eggs, cow’s milk, and fish being more prevalent in young children and peanuts, tree nuts, and shellfish being more common in older children and adolescents. Allergies to egg, milk and soy are often temporary, and children grow out of them. Allergies to peanuts, tree nuts, fish, and shellfish, on the other hand, are often life-long.
Diagnosing a food allergy can be challenging as there is no one test that can confirm or rule out this medical condition. Both skin prick tests and blood specific IgE tests are useful first line investigations for evaluation of suspected food allergies. Sometimes in patients with uncontrolled eczema, the results of these tests can be falsely positive. Therefore, these tools must be interpreted together with other medical information to confirm the diagnosis. Further investigations, such as component diagnosis or functional IgE assays available in specialist allergy centres, may be required in certain circumstances to confirm a food allergy, which will be discussed in detail in our next article.
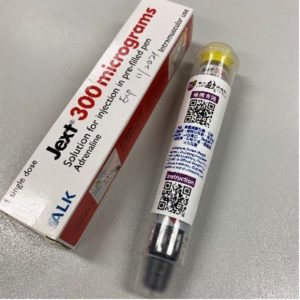
Food allergic reactions are unpredictable. Full avoidance of dietary allergens is difficult to achieve. According to data from the United States, approximately 40% of children with food allergies have had a severe or life-threatening reaction. The only medication that can treat anaphylaxis is epinephrine. Epinephrine, often known as adrenaline, is an injected medication that helps relieve the symptoms of a severe allergic response (Figure 1). While antihistamines can help ease certain minor allergic response symptoms, such as itchy tongue or hives, they cannot halt the potentially fatal symptoms of anaphylaxis. The best strategy for ensuring successful long-term care is still patient empowerment and education. Aside from educating the patient and his or her family on the proper care of severe food-allergic responses, such as the use of an adrenaline auto-injector, which is the first line therapy in all anaphylaxis reactions. Patients and parents should be taught how to read and interpret product ingredient labels in order to avoid cross-contamination with known allergens during meal preparation. Individuals should be encouraged to wear a medical identity bracelet and to ask about allergy exposure when dining out. The most successful way to enhance patient care and benefits is to implement structured patient educational programs that involve different health professionals including allergy specialists, nurses, dietitians, psychologists, pharmacists, patient organizations, and the food sector.
Please stay tuned to our next articles on the diagnostic strategies of food allergy and living with food allergy in the community. This year’s “CU Allergy Week” will be held from the 20th to the 27th May, 2023. It is an important initiatives of the CUHK Allergy team that aims to raise awareness of food allergy in Hong Kong. Education and knowledge will help people recognize allergic responses more quickly and efficiently respond to potentially life-threatening events. CU Allergy Week 2023 calls on all Hong Kong citizens to join our efforts in “Allergy Education: Every Child and Youth’s Right to a Healthy Life”.
References:
- Leung ASY, Li RMY, Au AWS, et al. Changing pattern of pediatric anaphylaxis in Hong Kong, 2010-2019. Pediatr Allergy Immunol 2022; 33: e13685. 20211031. DOI: 10.1111/pai.13685.
- Li P, Leung A, Li R, et al. Increasing incidence of anaphylaxis in Hong Kong from 2009 to 2019 — discrepancies of anaphylaxis care between adult and pediatric patients. Authorea July 21, 2020. DOI: 10.22541/au.159534865.55761541.
- Wai CYY, Leung NYH, Leung ASY, et al. Cell-Based Functional IgE Assays Are Superior to Conventional Allergy Tests for Shrimp Allergy Diagnosis. J Allergy Clin Immunol Pract 2021; 9: 236-244.e239. 2020/09/16. DOI: 10.1016/j.jaip.2020.08.057.


